OSTEOSARCOMA (OSTEOGENIC SARCOMA)
OSTEOSARCOMA (OSTEOGENIC SARCOMA)
- Second most common, and a highly malignant primary bone tumour.
- Pathology: An osteosarcoma can be defined as a malignant tumour of the mesenchymal cells, characterised by formation of osteoid or bone by the tumour cells.
Classification:
This tumour has been subclassified on the basis of:
- the clinical setting where it occurs; and
- its dominant histo-morphology
O/B of clinical setting, this tumour can be divided into primary and secondary.
1. Primary osteosarcoma, the commoner, occurs in the age group of 15-25 years.
- There are no known pre-malignant conditions related to it.
- It is very much more malignant than the secondary one.
2. The secondary osteosarcoma occurs in older age (45 years onwards).
Some of the pre-malignant conditions often associated with it are:
- Paget’s disease
- multiple enchondromatosis
- fibrous dysplasia
- irradiation to bones
- multiple osteochondroma etc.
Most osteosarcomas fall into the primary conventional category, and have the following important features.
1. Age at onset: occur b/w 15-25 years, constituting the commonest musculo-skeletal tumour at that age.
2. Common sites of origin: In decreasing order of frequency these are:
- the lower-end of the femur
- upper-end of the tibia; and
- upper-end of the humerus.
- However, any bone of the body may be affected.
3. Gross appearance of the tumour depends upon its dominant histo-morphology.
- An osteoblastic tumour is greyish white, hard, and has a gritty feeling when cut.
- A chondroid type may appear opalescent and bluish grey.
- A fibroblastic type has a more typical fish flesh sarcomatous appearance.
- The highly malignant, telangiectatic type may have large areas of tumour necrosis and blood filled spaces within the tumour mass.
- Most tumours have mixed areas.
4. Histologically, tumours vary in the richness of the osteoid, cartilaginous, or vascular components;
- but common to all is a basically anaplastic mesenchymal parenchyma with tumour cells surrounded by osteoid.
Clinical features:
- Pain is usually the first symptom, soon followed by swelling.
- Pain is constant and boring, and becomes worse as the swelling increases in size.
- There may be a history of trauma, but more often it is incidental and just draws the attention of the patient to the swelling.
- Sometimes, the patient presents with a pathological fracture.
Investigations:
Following investigations may be carried out to confirm the diagnosis:
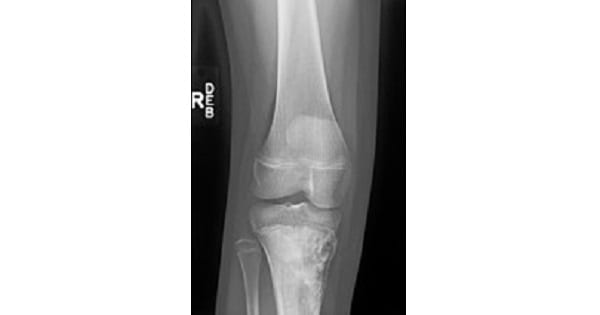
1. Radiological examination: X-ray shows the following features :
- An area of irregular destruction in the metaphysis, sometimes overshadowed by the new bone formation.
- The cortex overlying the lesion is eroded.
- There is new bone formation in the matrix of the tumour.
- Periosteal reaction: As the tumour lifts the periosteum, it incites an intense periosteal reaction.
- The periosteal reaction in an osteosarcoma is irregular, unlike in osteomyelitis where it is smooth and in layers.
- Codman’s triangle: A triangular area of subperiosteal new bone is seen at the tumour-host cortex junction at the ends of the tumour.
- Sun-ray appearance: As the periosteum is unable to contain the tumour, the tumour grows into the overlying soft tissues.
- New bone is laid down along the blood vessels within the tumour growing centrifugally, giving rise to a ‘sun-ray appearance’ on the X-ray.

2. Serum alkaline phosphatase (SAP):
- Generally elevated, but is of no diagnostic significance.
- Considered a useful parameter for follow up of a case of osteosarcoma.
- A rise of SAP after an initial fall after tumour removal is taken as an indicator of recurrence or metastasis.
3. Biopsy: An open biopsy is performed to confirm the diagnosis.
Treatment:
- The aim is to confirm the diagnosis, to evaluate spread of the tumour, and to execute adequate treatment.
Exam Important
- Calcification in osteosarcoma is due to presence of Osteoid matrix.
- Osteosarcoma commonly affects Metaphysis.
- Osteosarcoma is a ‘Pulsating tumor’ of the bone.
- Pre-malignant conditions often associated with Osteosarcoma are:
- Paget’s disease
- multiple enchondromatosis
- fibrous dysplasia
- irradiation to bones
- multiple osteochondroma
- Radiological feature of osteosarcoma is Sunray appearance & codmam triangle.
- Most common site of osteosarcoma is lower-end of the femur.
- Methods used for evaluation of Osteosarcoma are : bone scan for finding the intra-medullary spread (‘skip’ lesions), CT and MRI scans for finding the soft tissue spread.
- Osteosarcoma is radioresistant.
- Retinoblastoma is associated with Osteosarcoma.
- Histology of Myositis ossificans mimics Osteosarcoma.
- Osteosarcoma is Least likely to regress spontaneously.